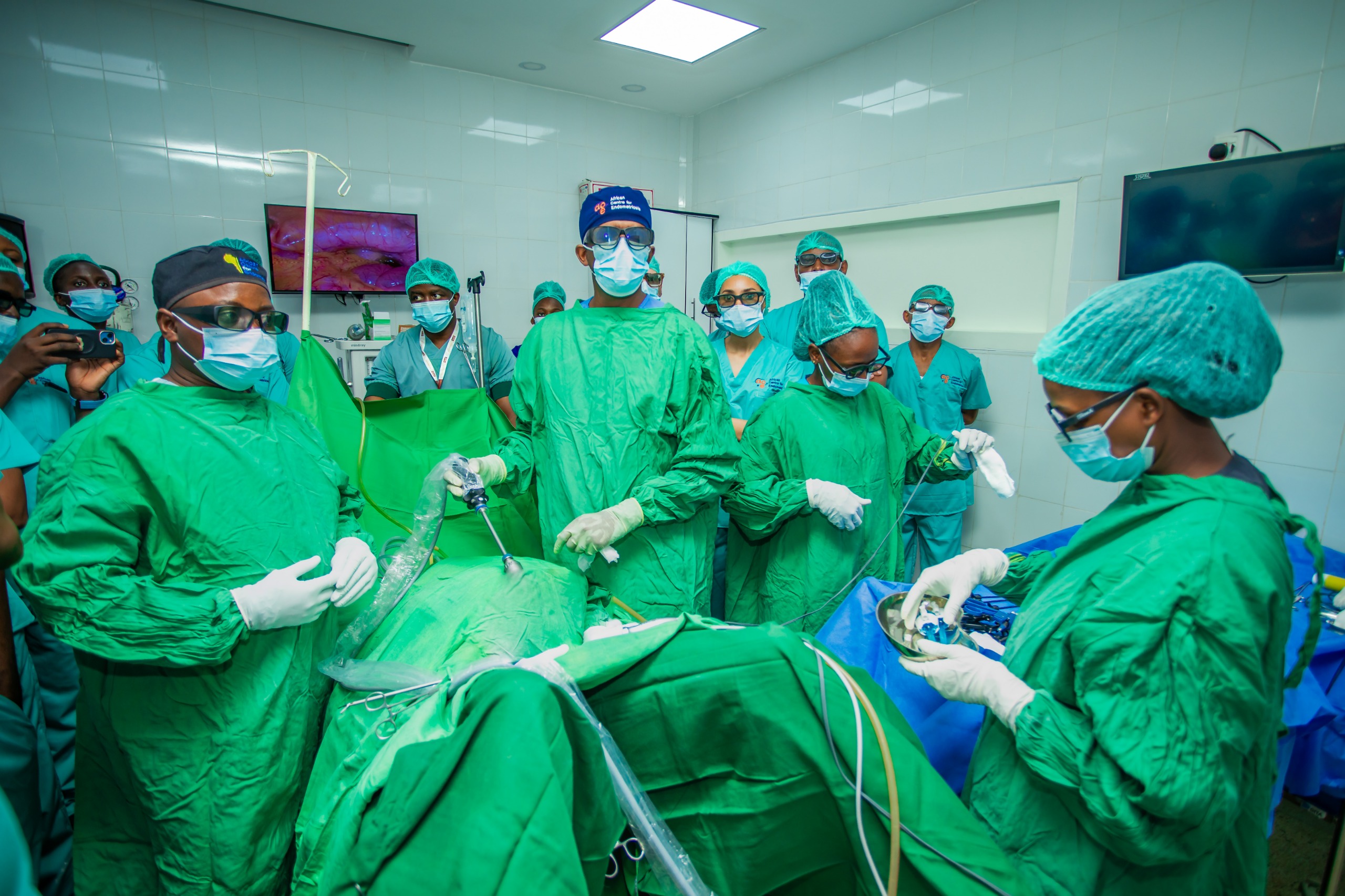
 A team of doctors doing a minimally invasive surgery on an endometriosis patient during the Healing Mama Africa bootcamp at Mt. Kenya hospital in Kerugoya on March 17, 2026/ ALICE WAITHERA
A team of doctors doing a minimally invasive surgery on an endometriosis patient during the Healing Mama Africa bootcamp at Mt. Kenya hospital in Kerugoya on March 17, 2026/ ALICE WAITHERAIn 2017, Jackline Njeri began experiencing unexplained chest pains that gradually worsened, eventually affecting her breathing.
The pain followed a pattern and intensified during her menstrual cycle and eased afterwards but at the time, she did not connect the symptoms to a reproductive health condition.
Over time, the episodes became more severe, accompanied by persistent headaches and debilitating cramps that disrupted her daily life.
Njeri, who hails from Kagio in Kirinyaga county, sought medical attention and was diagnosed with tuberculosis.
She was placed on medication for six months, but her symptoms did not improve. Concerned, she returned to the health facility and was prescribed another six-month course of treatment, which she diligently completed.
Still, the pain persisted. Doctors later concluded she had developed drug-resistant tuberculosis and placed her on an even longer treatment regimen lasting about 18 months.
Despite years of treatment, her condition showed no signs of improvement. Frustrated and physically drained, Njeri sought a second opinion.
This decision marked a turning point. She was referred to a specialised endometriosis facility in Kerugoya, where she was finally diagnosed with thoracic endometriosis, a rare form of the condition that affects the chest cavity.
Endometriosis is a chronic, often painful diseases where tissue similar to the lining of the uterus grows outside the uterus, causing inflammation and scar tissue.
Njeri underwent surgery last year.
“Since the surgery, my life has taken a turn. There’s no more pain and discomfort and I’m now able to go about my life like anybody else,” she said.
However, the long journey to diagnosis and treatment had already taken a toll on her social life and finances.
The surgery cost about Sh1.3 million, with the Social Health Insurance Fund covering only Sh300,000, leaving her with a significant financial burden.
Njeri shared her experience during the Healing Mama Africa Boot Camp, a five-day medical outreach held at Mt Kenya Hospital.
The initiative brought together local and international specialists to offer treatment and raise awareness about endometriosis, a condition that continues to be widely misunderstood and underdiagnosed across Africa.
Among the attendants was Lacroix Tope, a young woman from Nigeria who had struggled with severe menstrual pain for years.
Like many others, she had lived with worsening symptoms and little relief.
“I have struggled with extreme cramps for many years and the pain just got worse and worse,” she said.
Her journey to Kenya began after discovering Dr Joe Njagi, an endometriosis specialist and advanced minimally invasive gynaecological surgeon, through social media.
 Dr Joe Njagi, an endometriosis specialist and advanced minimally invasive gynaecological surgeon, during the Healing Mama Africa bootcamp in Kerugoya on March 17, 2026 /ALICE WAITHERA
Dr Joe Njagi, an endometriosis specialist and advanced minimally invasive gynaecological surgeon, during the Healing Mama Africa bootcamp in Kerugoya on March 17, 2026 /ALICE WAITHERANjagi has been actively raising awareness about the condition online, helping patients across borders access care.
Arrangements were made for Tope to travel to Kenya, where she is now set to undergo surgery in the hope of ending years of pain.
Njagi said the boot camp had attracted patients from across the continent, including countries such as Cameroon, highlighting the widespread demand for specialised care.
“This week, we’re going to perform 103 ultrasound scans and conduct at least 20 endometriosis surgeries,” he said.
However, Njagi emphasised that such initiatives should go beyond treatment camps and serve as a catalyst for long-term change.
“This initiative should act as a platform for awareness, a call to improve our practices, train more specialists and be intentional about enhancing care for endometriosis and related conditions,” he said.
Njagi said misdiagnosis remains a major challenge, with many patients undergoing prolonged and often unnecessary treatments.
Some, like Njeri, are treated for other conditions such as tuberculosis due to overlapping symptoms.
Njagi said thoracic endometriosis can present with chest pain, coughing and fluid accumulation in the chest cavity, particularly during menstruation, symptoms that can easily be mistaken for respiratory illnesses.
“These are patients who experience chest pain, coughing or fluid in the chest every month during their menses. Without specialised knowledge, it’s easy to misdiagnose them,” he said.
Njagi said endometriosis can affect multiple organs, including the diaphragm, lungs, intestines, bladder, urethra and even kidneys, making diagnosis and treatment complex. In severe cases, delayed diagnosis can lead to irreversible damage.
“One of the patients we’ll operate on this week lost a kidney due to endometriosis. Others have suffered infertility,” he said.
Globally, one in 10 women is estimated to suffer from endometriosis, with about six per cent of Kenyan women affected.
However, the lack of comprehensive data in Africa has hindered effective interventions, contributing to delayed diagnoses that can take between 10 and 20 years.
Access to treatment remains another significant barrier. Njagi pointed out that endometriosis care, especially surgical intervention, is expensive and requires a multidisciplinary team.
Patients often need coordinated care involving gynaecologists, surgeons, radiologists and other specialists, depending on the organs affected.
“There are very few facilities offering comprehensive endometriosis treatment, which limits access for many patients,” he said.
“That’s why initiatives like Healing Mama Africa are important—they bring services closer to underserved populations.”
 Prof Ahmed Minawi, an endometriosis specialist and a gynaecologic endoscopy and robotic surgery consultant addressing attendants during the Healing Mama Africa bootcamp at Mt Kenya Hospital in Kerugoya on March 17, 2026 /ALICE WAITHERA
Prof Ahmed Minawi, an endometriosis specialist and a gynaecologic endoscopy and robotic surgery consultant addressing attendants during the Healing Mama Africa bootcamp at Mt Kenya Hospital in Kerugoya on March 17, 2026 /ALICE WAITHERADr Yamal Patel, another specialist at the camp, highlighted the psychological toll of the condition, noting that prolonged suffering and lack of diagnosis can push some patients to the brink.
“This is not just any disease. It disrupts lives completely. Many patients develop severe emotional distress after years of seeking help without answers,” he said.
Prof Ahmed Minawi, an endometriosis specialist, said the Pan-African Society of Endometriosis, established in 2024, is working to address gaps in knowledge and care.
The organisation held its first conference in South Africa and plans to host a global conference in Mombasa next year.
He said Africa continues to struggle with underdiagnosis and lack of reliable data. Even in countries with long-established medical institutions, such as Egypt, official statistics on endometriosis remain scarce.
This has allowed the condition to persist in silence, compounded by stigma surrounding menstruation and menstrual pain.
Dr Orora Maranga, a gynaecologic oncologist at Kenyatta National Hospital, said the challenges facing women’s health in Kenya extend beyond endometriosis and reflect broader systemic gaps.
He said limited specialist numbers, high patient volumes and constrained resources continue to hinder effective care.
Kenya has a doctor-to-population ratio of just 0.2 physicians per 1,000 people, far below global recommendations.
At the same time, the country faces a growing burden of non-communicable diseases, including cancer, which disproportionately affects women.
Breast, cervical and colorectal cancers are among the leading causes of illness with nearly 60 per cent of cases occurring in people under the age of 70.
Further, more than 70 per cent of cancer cases in Kenya are detected at advanced stages, significantly reducing treatment success rates.
Screening uptake is also low with fewer than 17 per cent of eligible women ever screened for cervical cancer and only about one per cent undergoing mammography for breast cancer.
Access to treatment is further complicated by infrastructure and financial constraints. The country has only about 19 external beam radiotherapy machines for a population of more than 50 million, falling short of international recommendations.
Public hospitals such as KNH face frequent equipment breakdowns and shortages of essential drugs, leading to delays in care.
Cost of treatment places an additional burden on patients and their families. On average, households spend up to Sh3.8 million annually on cancer care, covering surgery, chemotherapy and radiotherapy.
Although recent reforms under the Social Health Authority have increased coverage to Sh800,000 per household, many patients still face significant out-of-pocket expenses.
“These financial pressures often force patients to abandon treatment or delay seeking care altogether,” Dr Maranga said, adding that up to 40 per cent of patients are lost to follow-up due to cost and access challenges.
Despite these hurdles, there have been notable advancements. The government has introduced the National Cancer Control Strategy and expanded access to specialised services.
New technologies, such as advanced radiotherapy systems, are also being deployed to improve treatment outcomes.
Instant Analysis
Globally, one in 10 women is estimated to suffer from endometriosis, with about six per cent of Kenyan women affected. Lack of comprehensive data in Africa has, however, hindered effective interventions, contributing to delayed diagnoses that can take between 10 and 20 years.






Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!