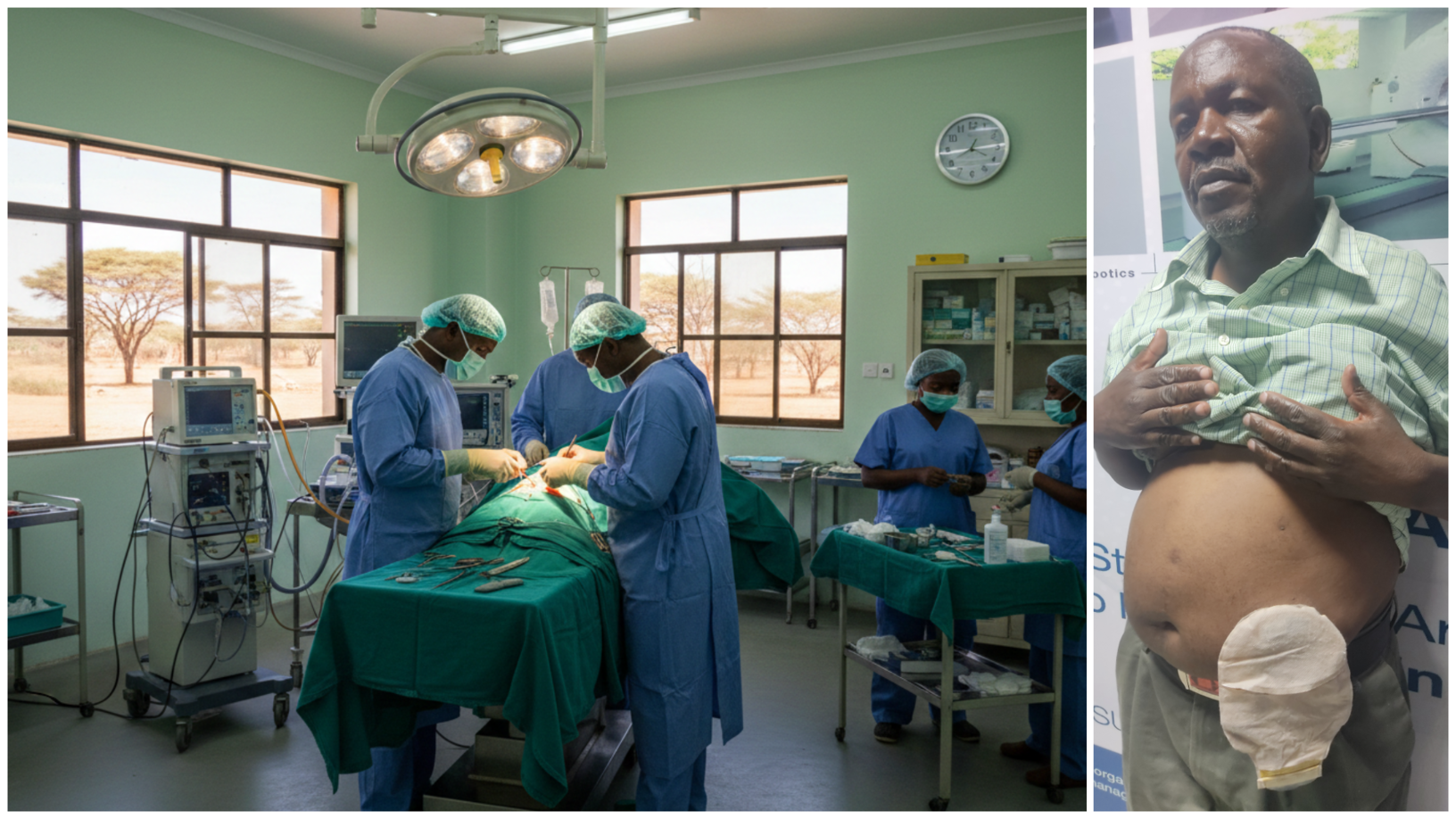
 Six of 10 surgeries James Gitonga has undergone were botched / AI AND CLARET ADHIAMBO
Six of 10 surgeries James Gitonga has undergone were botched / AI AND CLARET ADHIAMBOAfter enduring six botched surgeries in reputable public and private hospitals locally,James Gitonga has vowed never to seek treatment from a Kenyan hospital again.
The procedures not only left him in chronic pain and damaged his anal sphincter but also impoverished him, stripped him of his dignity and nearly destroyed his marriage.
Of the 10 surgeries Gitonga has had, six were botched.
In one of the botched procedures, a surgeon at a private hospital in Nairobi removed the clips from his surgical wound, which was oozing greyish discharge, left his abdomen open, went home and switched off his phone.
“I think he panicked and didn’t know what to do when the wound started oozing grey matter. We tried calling him but he refused to pick up his phone. The nurses at the hospital also refused to touch me,” Gitonga told the Star.
Trouble began in 2016, when James started experiencing persistent itching around the anus. He had previously undergone surgery in 2008 to treat haemorrhoids.
“I was in Sudan when the itching started, but I assumed it was a result of the previous haemorrhoid surgery,” he said.
Unfortunately, war broke out in Sudan, forcing Gitonga to return to Kenya to rebuild his life. But the itching persisted.
He started self-medicating, taking anti-haemorrhoid drugs, but the pain did not subside. Eventually, he reached out to a friend who is a clinical officer.
“He examined me and told me I did not have haemorrhoids,” Gitonga said.
PHYSICAL, MENTAL TRAUMA
The friend referred him to a hospital in Kikuyu for a procedure that would ultimately trigger a series of botched surgeries and a long, agonising search for healing.
By the time he arrived at the hospital, he was in excruciating pain and unable to sit.
“They told me they will take me to theatre, open me up and see what the problem is.” Consultation alone cost Gitonga Sh20,000.
The following day, two doctors, a senior female and a junior male, wheeled him to theatre.
Midway through the procedure, the senior doctor was called for an emergency, leaving the junior doctor alone.
“I think the young doctor messed me up. After he finished, the lady doctor returned and asked him what he had found. He said, ‘I saw some pus and drained it. I don’t think you have any other problem,’” Gitonga recounted.
The senior doctor appeared dissatisfied and started scolding him, repeatedly asking, “What have you done?”
From that exchange, Gitonga suspected that something had gone wrong during the surgery.
The doctors kept him hospitalised for two more days before discharging him. As if to cover their backs, the hospital refused to issue a discharge summary.
“I was in a lot of pain when they discharged me, and they did not give me a single document to show I had been admitted,” he said.
A few days later, his left buttock started to swell. His sisters moved him to his mother’s house to manage the condition as his wife was away for work.Soon, he was unable to pass stool. Shortly afterwards, another hole formed near his anus, oozing blood.
The swelling worsened and Gitonga lost control of his sphincter muscle, leaving him unable to control his bowel movements.
“My family bought me adult diapers to manage the situation. When the pain became unbearable and I could not sleep, they took me to another doctor who ran a private clinic,” he said.
After several tests and a physical examination, Gitonga was informed that doctors at the Kikuyu hospital had created a fistula and he needed corrective surgery.
Because the doctor did not have a theatre at his clinic, he transferred Gitonga to another private hospital in Mwea, Kirinyaga county, where he was charged about Sh100,000 for surgery.
Two days later, however, the wound swelled again and burst.
“Out of fear, I called my sister from the hospital and told her what I was experiencing. I warned her I might become septic,” Gitonga said.
His family cleared the hospital bill and arranged for an ambulance to transfer him to a top private hospital in Nairobi.
After examination, a team of surgeons concluded that he required reconstructive surgery, including the creation of a diverting stoma to stabilise his condition.
First, they created the stoma, bringing part of his intestine to the abdominal surface and attaching a colostomy bag.
FROM BREADWINNER TO BEGGAR
Three months later, Gitonga returned for reconstructive surgery.This time, he was placed under general anaesthesia.
Unfortunately, a nerve stimulator malfunctioned mid-procedure, necessitating yet another surgery.
“I was deeply disappointed. Surgeries are not only extremely painful but also financially draining. I asked God many questions,” he said.
The doctor, however, remained optimistic and recommended plastic surgery at a renowned public hospital.
The plastic surgeon recommended reversing the stoma afterwards at a private hospital. However, the procedure backfired.
By this time, Gitonga was financially drained and had started relying on harambees to cover his medical expenses.
Despite an empty bank account, his resolve was clear: raise the required amount and get better.
“The stoma reverse surgery was very painful. For about six or seven days, I was not allowed to eat and was fed through tubes,” he said.
Unfortunately, while recovering at the hospital, the Covid-19 pandemic struck, and around that time, Gitonga became feverish.
He says the fever sent the hospital into panic mode. He was removed from the ward and placed in isolation.
For four days, Gitonga saw no doctor, only Kenya Medical Research Institute personnel who came to collect swabs for Covid-19 tests.
“Only I know what I went through. It was the worst period of my life. They stopped treating me and shifted all focus to Covid, yet I was in extreme pain,” he said.
After four days, he tested negative and was taken back to the ward.
One morning, while still in the ward, a clear substance started to leak from the stoma wound. When the surgeon visited, he asked whether Gitonga was diabetic. He said he was not.
The surgeon then removed the surgical clips, left his abdomen open and switched off his phone.
Gitonga says he stayed the entire day with an open abdomen.
“Some of my family members fainted when they saw me in that condition. I thought I was dying. I demanded to be discharged so I could go and die in a public hospital,” he said.
At the public hospital, even the most senior surgeons declined to handle his case.
Eventually, another friend referred him to a doctor who proposed reinstating the stoma while attempting to assess the underlying problem.
After surgery, the doctor informed him that the condition was highly complex and suggested seeking specialised treatment in India.
By then, Gitonga had sold his land and car. He struggled to pay school fees and his marriage was crumbling.
“My children stayed home for days because of unpaid school fees. My wife even moved out of our bedroom because of the indignity of living with a colostomy bag,” he said.
Beyond the physical pain, he endured public humiliation.
“The anal opening sometimes releases clear fluid that stains my trousers. On my way to this interview, I soiled myself. I just hoped it would dry and kept walking,” he said.
SH4M HOPE IN INDIA
A friend later connected him to Pathway International, an organisation that links patients to specialists in India.
After reviewing his reports and conducting tests, specialists from Apollo Proton Cancer Centre in India concluded that his sphincter muscle had been severely damaged.
They recommended specialised therapy to repair the muscle.
“They said if the damage is less than 60 per cent, they could repair it. If it exceeds 60 per cent, they would consider a transplant,” John Kibe of Pathway International said.
To undergo treatment, Gitonga needs about Sh4.1 million to cover surgery, medication, travel, food and accommodation.
Gitonga’s case of botched surgeries in Kenya is not isolated. In 2018, doctors at a reputable public hospital performed brain surgery on the wrong patient.
In January, a man died in Kawangware after a botched tooth extraction.
To enhance surgical safety globally, the World Health Organisation introduced the WHO Surgical Safety Checklist in 2008, a 19-item tool designed to
improve adherence to standards of care and strengthen team communication.
The checklist has significantly improved surgical outcomes in many settings, though most evidence comes from high-income countries.
In low-income countries, implementation and impact remain inadequately documented.
In Kenya, most healthcare workers are aware of the checklist and use it, though not consistently.
Despite its simplicity, the checklist is intended to reduce human error and enhance patient safety in operating theatres.
In March last year, Lifebox, an NGO, conducted WHO Surgical Safety Checklist training for 18 nurses, surgeons and anaesthesia professionals from public and private hospitals.
Gitonga’s ordeal is more than a personal tragedy. It is a stark indictment of a health system where surgical errors can spiral into lifelong disability, financial ruin and emotional devastation.
“All I need right now is to get better,” he says. “I would not want to sue the hospitals because even if I did, who would admit liability from the series of botched surgeries?”
To help Gitonga, you can reach out to him on 0700386856 or Pay Bill number 247247 Account number 0010101204247.






Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!