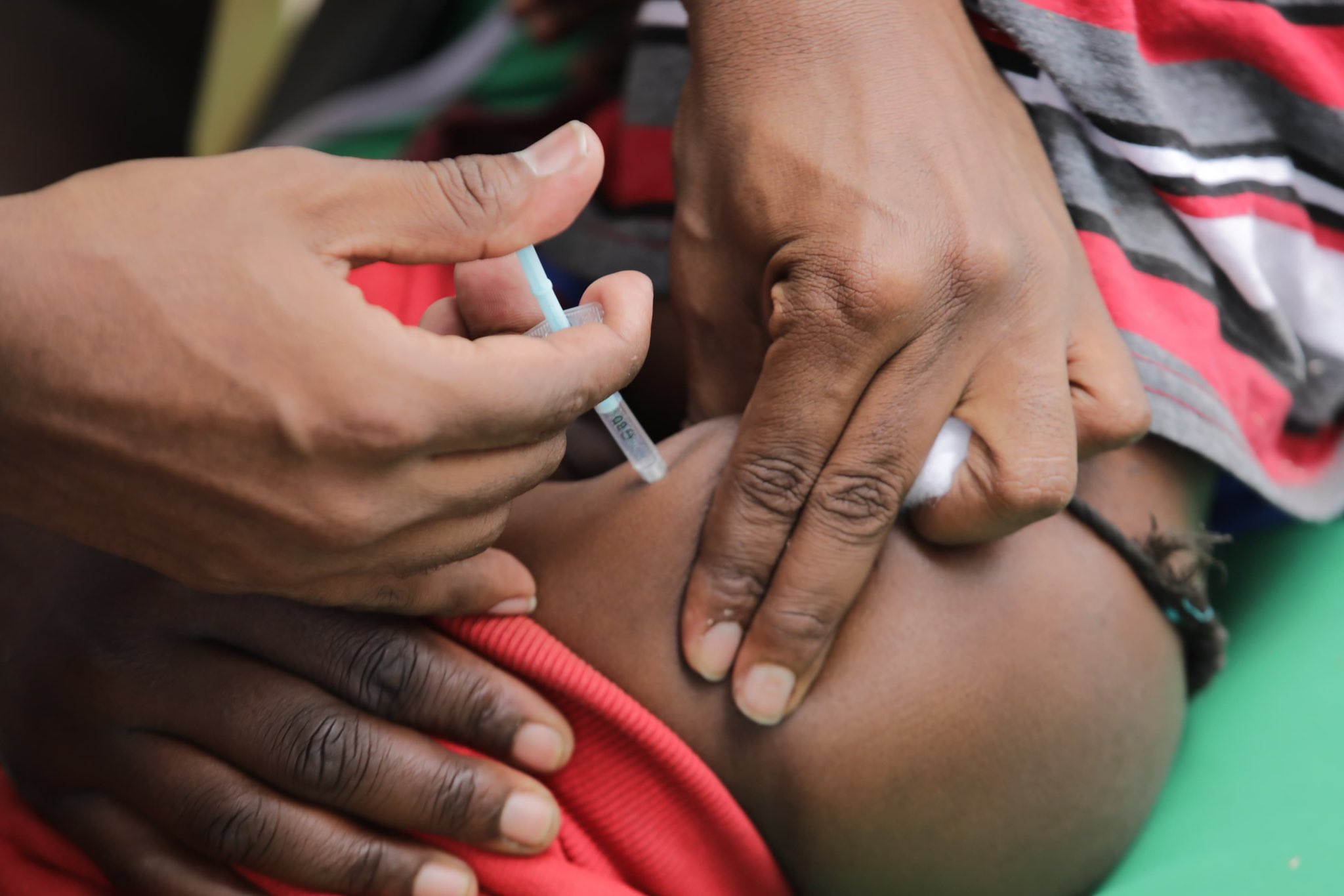
 A healthcare worker administers a vaccine to a child during the ongoing Measles-Rubella and Typhoid Conjugate Vaccine (TCV) campaign, July 12, 2025 /MoH
A healthcare worker administers a vaccine to a child during the ongoing Measles-Rubella and Typhoid Conjugate Vaccine (TCV) campaign, July 12, 2025 /MoH
Nearly 20 million measles-related deaths have been averted in Africa, including thousands in Kenya, since 2000, thanks to increasing vaccination coverage, according to the first-ever detailed analysis of immunisation targets on the continent.
Progress on measles underscores the impact of consistent investment in immunisation.
Since 2000, 44 African countries have introduced a second dose of measles-containing vaccine into routine immunisation, helping to increase coverage rates from five per cent in 2000 to 55 per cent in 2024.
Supplemental campaigns have delivered 622 million vaccinations. These efforts collectively have halved measles deaths in the African region and led to a 40 per cent drop in overall cases.
In Kenya, measles vaccination coverage remains below the 95 per cent threshold needed to stop transmission.
Recent estimates show that about 91 per cent of children receive the first dose, but only around 76 per cent complete the second dose, leaving a significant immunity gap.
This drop-off has contributed to recurring outbreaks, with nearly 3,000 cases and multiple deaths reported between 2024 and early 2025, and low uptake of the second dose has been identified as a key driver of vulnerability across several counties.
While the region has made huge progress towards protecting populations from measles, some countries have gone further.
In 2023 and 2024, nine countries reported consistently low measles incidence rates (fewer than five cases per million).
Last year, Cabo Verde, Mauritius and Seychelles became the first sub-Saharan African countries to achieve measles and rubella elimination status, the gold standard in protecting against both diseases.
The analysis also assessed overall progress and challenges in expanding immunisation coverage against a broad range of diseases, as well as ongoing efforts to reach the targets of the 2030 Immunisation Agenda—a global strategy to reduce vaccine-preventable deaths and diseases, expand vaccine access and strengthen immunisation within primary healthcare.
Routine immunisation schedules currently protect against 13 vaccine-preventable diseases, up from eight in 2000; meningitis deaths have fallen by 39 per cent; malaria vaccine has been introduced in 25 countries; and in 2024 alone, at least 1.9 million lives were saved through vaccination—42 per cent of which were due to measles vaccination.
“Africa has made remarkable progress in less than a generation, expanding immunisation and saving millions of young lives,” Dr Mohamed Janabi, WHO regional director for Africa, said.
“But the progress is uneven, and even slowing, leaving too many children unprotected as key targets are still missed. We must urgently strengthen routine immunisation to leave no child behind.”
Additionally, 47 sub-Saharan African countries now provide hepatitis B as part of routine vaccination, with 16 countries providing a birth dose; 33 have introduced the rubella vaccine; and 29 countries offer the human papillomavirus vaccine, which protects against cervical cancer.
“This analysis highlighting 24 years of remarkable progress on the African continent demonstrates the immense life-saving power of vaccines when immunisation is prioritised as a matter of policy,” Dr Sania Nishtar, CEO of Gavi the Vaccine Alliance, said.
“At the same time, we must acknowledge that these immunisation outcomes reflect very different realities, and we have more work to do to ensure we are consistently able to reach children, even in the most fragile and remote contexts.
“Through the Gavi Leap reform agenda, we hope to unlock further progress through novel, innovative approaches and by working with countries to build sustainable, self-reliant programmes for the long term.”
The analysis by WHO and Gavi plays a critical role in providing evidence to support policy formulation as well as assessing and understanding the impact of investments towards Immunisation Agenda 2030 targets in the region.
The Immunization Agenda 2030 aims for 90 per cent coverage of four key life-stage vaccines: the third dose of the diphtheria, tetanus toxoid and pertussis vaccine (DTP3); the third dose of the pneumococcal conjugate vaccine (PCV3); the second dose of the measles-containing vaccine (MCV2); and one dose of the human papillomavirus vaccine (HPV).
Although millions more children are being vaccinated and efforts to reduce the number of unvaccinated children are proving successful, Africa is off track towards the 90 per cent coverage target, as immunisation coverage is uneven and a large number of children—often those that are the hardest to reach—are still being missed, worsening immunisation equity within countries.
Rapid population growth, weak health systems, lack of integration of immunisation programmes in primary health care, as well as the devastating impact of climate change, humanitarian crises and political instability are some of the major hurdles to reaching the optimal vaccination coverage.
Continued investment by countries and strong political commitment are critical to sustain gains and protect future generations.
Focus on building or rebuilding resilient immunisation systems at the sub-national level is central to containing prevalent immunisation inequities and sustaining coverage at no less than 90 per cent.
WHO, Gavi and partners are working with governments to widen vaccination coverage as well as accelerate and scale up the introduction of new vaccines such as those for malaria and human papillomavirus.








Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!