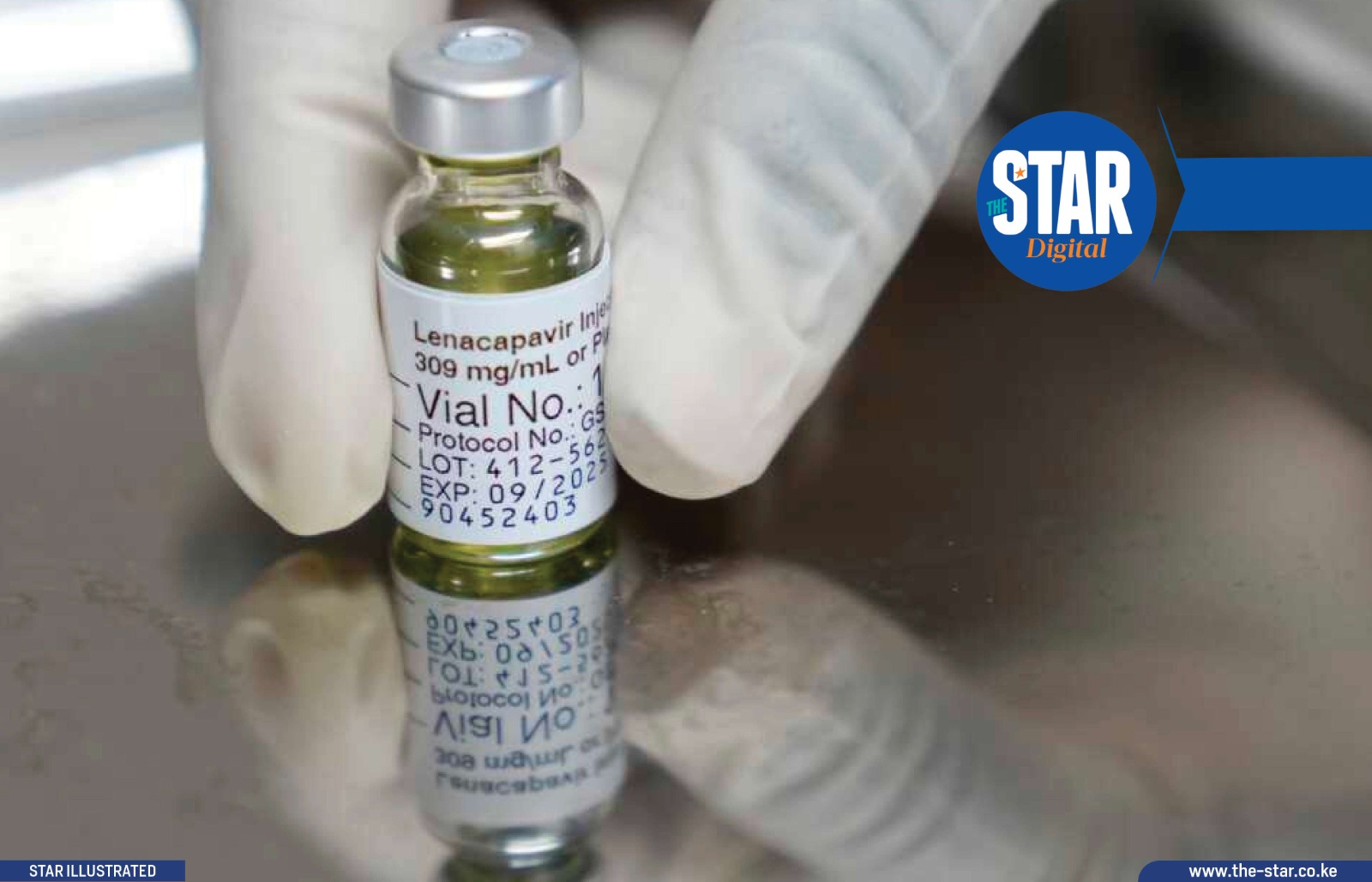
 Lenacapavir: Kenya's new HIV prevention medicine
Lenacapavir: Kenya's new HIV prevention medicineLong-acting injectable lenacapavir, which will be launched in Nairobi on Thursday, has emerged as one of the most powerful new tools in HIV prevention.
The drug, also called LEN, is injected under the skin of the abdomen once every six months to prevent HIV in a negative person.
Amref Health boss Dr Gitahi Githinji moved to quell the excitement, saying it does not override other prevention methods even if you get the injection. During trials, two people who got the shot still got infected with HIV.
"Lenacapavir is not a substitute for comprehensive HIV prevention strategies. Continue to practice safe sex, including consistent and correct condom use, and other prevention methods as advised by your healthcare provider," he said.
"Lenacapavir is not a replacement to long term HIV treatment for those living with HIV, nor is it a vaccine - it’s a pre-exposure injection for those negative but are at high risk of infection," he added.
Each injection contains just one to 2 mL of liquid, manufacturers say. This is a small amount that can fit inside a bottle cap.
The drug works by blocking a key outer shell of the HIV called the capsid, which the virus needs to enter human cells and multiply. Blocking this shell, it stops HIV from taking control of your body’s immune cells and spreading.
The main trials that prove the drug prevents HIV infection were called PURPOSE 1 and PURPOSE 2, and were conducted between 2021 and 2024.
In the PURPOSE 1 study, 5,338 girls and young women (16-26 years) in South Africa and Uganda, who were HIV-negative, were randomly assigned to receive either lenacapavir injections every six months or daily oral PrEP (TDF/FTC).
In the PURPOSE 2 study, 3,267 HIV-negative men and women above 16 years in Argentina, Brazil, Mexico, Peru, South Africa, Thailand and the United States were randomly assigned in a 2:1 ratio. This means two people received lenacapavir injections for every one person who received daily oral TDF/FTC.
There was no placebo in any group because oral PrEP is already proven effective, so researchers compared how many people in each group became infected over time, while also closely monitoring safety.
“PURPOSE 1 trial…demonstrated LEN’s efficacy in preventing HIV among cisgender women in sub-Saharan Africa, with zero infections among women receiving the injectable,” the World Health Organization reported in September 2024.
In the Purpose 2 study, among the 2,180 people who received lenacapavir, only two new HIV infections were recorded. That means 99.9 per cent of those using LEN did not acquire HIV.
In comparison, nine new infections occurred among 1,087 participants who took daily oral TDF/FTC.
The WHO said the results from PURPOSE 1 and PURPOSE 2 provide compelling evidence that LEN actually prevents HIV.
“LEN’s twice-yearly dosing offers a significant advantage for people who face challenges with adhering to daily oral PrEP, including stigma and discrimination, pill fatigue, and challenges with consistent access to medication,” WHO said.
Despite the near-perfect protection rates, experts are closely examining the two breakthrough infections recorded in PURPOSE 2.
According to the WHO’s evidence review, both individuals who acquired HIV while receiving lenacapavir had a specific mutation associated with resistance to HIV-1 capsid inhibitors. The mutation is known as N74D.
This raises an important scientific question. Could the use of lenacapavir select for virus strains that are resistant to this new drug class?
WHO has described the certainty of evidence on resistance as low, but has emphasised that ongoing monitoring will be critical as the drug is rolled out more widely. Lenacapavir is the first capsid inhibitor approved for prevention, meaning there is currently no widespread background resistance in the population.
Still, resistance surveillance will matter. If breakthrough infections occur, early detection and rapid linkage to effective treatment will be essential to prevent onward transmission of the resistant virus.
Importantly, two infections out of more than two thousand participants still reflect extremely high protection.






Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!