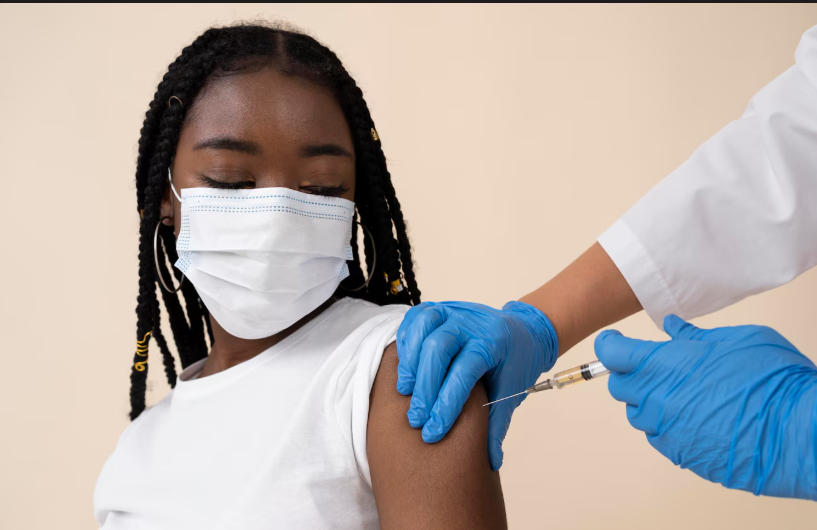
January is Cervical Cancer Awareness Month, a global campaign highlighting prevention, early detection, and treatment of one of the leading causes of cancer-related deaths among women.
In Kenya, Kenyatta National Hospital (KNH) has used the month to stress that cervical cancer prevention is not solely a women’s issue, noting that men play a critical and often overlooked role in the spread and prevention of human papillomavirus (HPV), the virus responsible for most cervical cancer cases.
The World Health Organization (WHO) describes HPV as a common sexually transmitted infection, stating that almost all sexually active people will be infected at some point, usually without symptoms.
In a public health message during the awareness month, KNH urged men to participate actively in cervical cancer prevention by getting vaccinated against HPV, highlighting that men often carry and transmit the virus asymptomatically.
Vaccinating men, the hospital said, protects their partners and reduces transmission in the wider population.
A medical specialist at KNH described HPV vaccination as a shared responsibility, not an intervention targeting women alone. She encouraged men to get the vaccine, noting they may unknowingly transmit the virus to their partners.
“Men play a vital role in cervical cancer prevention by encouraging their partners, female friends, and sisters to go for screening. All men should also get the HPV vaccine because they may be asymptomatic carriers. Vaccination is important for everyone,” she said.
The specialist added that vaccination remains one of the most effective tools against HPV-related cancers and urged the public to use available services.
KNH offers HPV vaccination, including for girls, and HPV DNA testing to detect high-risk HPV types that can lead to cervical cancer if untreated. Early detection through screening, she said, significantly reduces the risk of invasive cancer.
The hospital also cautioned against stigma, stressing that HPV infection or a cancer diagnosis should not be linked to sexual immorality.
The specialist explained that even faithful partners can contract HPV, as the virus is common and can remain undetected for years.
“Having HPV or cancer does not necessarily mean someone has been unfaithful. A person can be faithful, and the partner may also be faithful, yet still contract the virus,” she said.
She urged focus on education and prevention rather than blame, warning that stigma discourages screening and treatment.
The specialist called for increased sensitisation, safe sex practices, adoption of new research findings, and routine screening. KNH stressed that public health messaging should extend beyond HIV prevention, noting that HPV is equally serious and causes multiple cancers.
“It’s not just HIV we need to be concerned about; HPV is also serious and can cause cancer. The good news is that it can be prevented,” she said, adding that HPV-related cancers are preventable through vaccination and screening, which remain more effective and affordable than treatment.
According to WHO, HPV affects the skin, genital area, and throat. Most infections clear on their own, but persistent infection with high-risk HPV types can cause cancer. In about 90 per cent of cases, the immune system controls the infection within one to two years without lasting effects.
“Persistent HPV infection with high-risk types causes cervical cancer and is associated with cancers of the vulva, vagina, mouth/throat, penis, and anus,” the agency notes.
Globally, WHO estimates HPV caused about 620,000 cancer cases in women and 70,000 in men in 2019. Cervical cancer typically develops 15 to 20 years after HPV infection.
“Cervical cancer is the most common HPV-related cancer; other less common cancers affect men and women, including anal, vulvar, vaginal, mouth/throat, and penile cancers,” WHO reports.
The agency states that HPV vaccination is the most effective preventive measure.
In 2022, cervical cancer ranked fourth among cancer causes and deaths in women, with around 660,000 new cases and 350,000 deaths globally.
WHO data show the highest prevalence of cervical HPV infection among women is in sub-Saharan Africa, estimated at 24 per cent, followed by Latin America, the Caribbean, Eastern Europe, and South-East Asia.
The burden is highest in low- and middle-income countries due to limited vaccination, screening, treatment, and broader social and economic inequalities.
HPV can also cause cancers of the vulva, vagina, anus, penis, and mouth and throat, affecting both men and women.
Currently, WHO notes that cervical cancer is the only HPV-related cancer with available screening tests, which detect precancerous changes before they progress, allowing treatment to prevent disease.
WHO recommends women start screening at age 30, every five to ten years, with women living with HIV screened more frequently from age 25.
As part of its global strategy, WHO aims to eliminate cervical cancer as a public health problem, targeting 90 per cent HPV vaccination coverage among girls by age 15, 70 per cent screening coverage among women by ages 35 and 45, and 90 per cent treatment coverage for women diagnosed with cervical disease.
As January Cervical Cancer Awareness Month ends, KNH and WHO urge the public to view cervical cancer prevention as a collective effort, with men and women equally participating in vaccination, screening, education, and the fight against stigma to reduce HPV transmission and save lives.





Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!