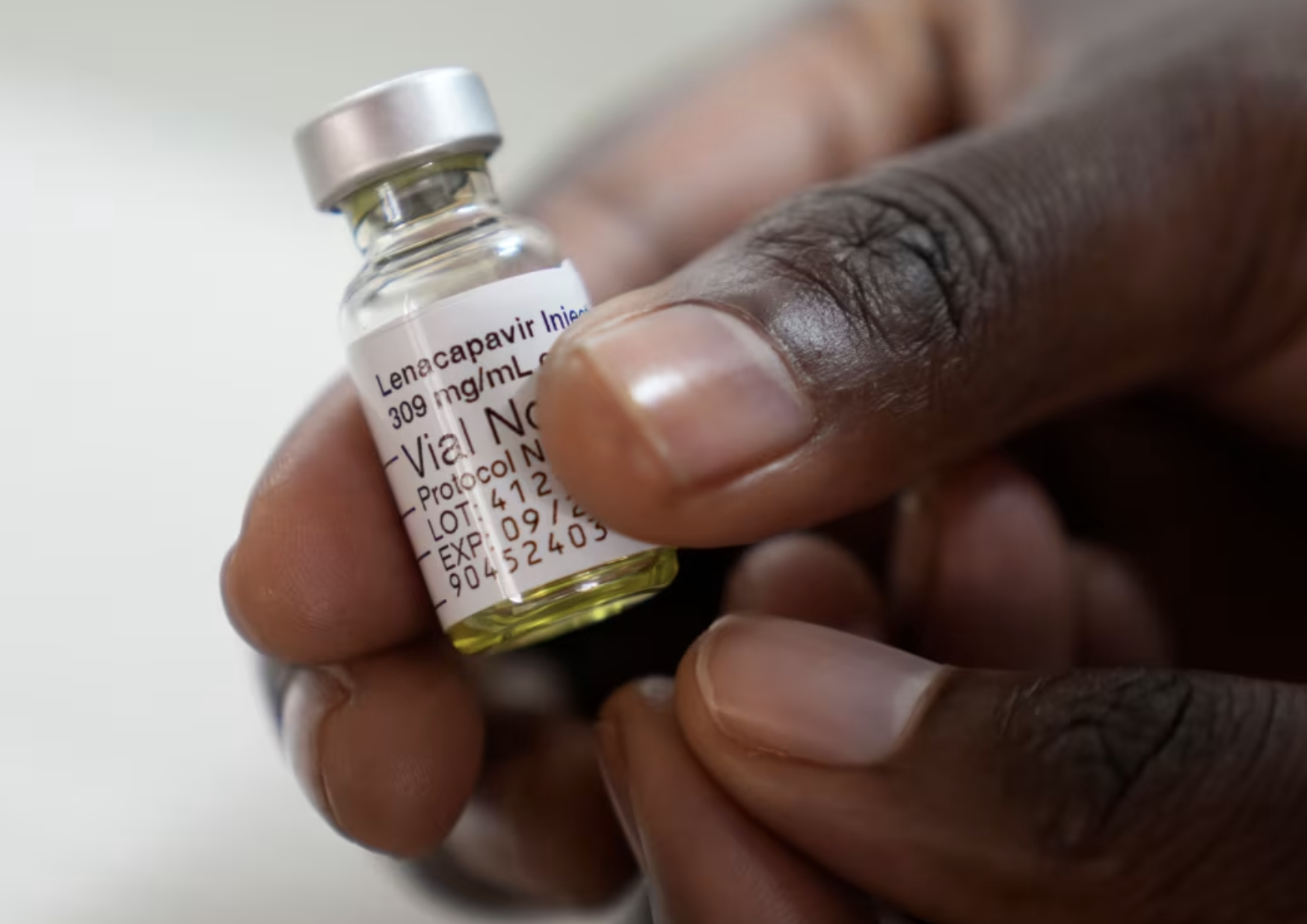
The introduction of a revolutionary drug, Lenacapavir, is poised to alter the landscape of healthcare across sub-Saharan Africa, where the HIV burden remains highest.
Kenya, with an estimated 1.4 million people living with HIV, stands to benefit significantly from the drug’s unique formulation and long-acting delivery.
Lenacapavir, developed by Gilead Sciences, is a long-acting antiretroviral drug that works differently from existing HIV medications.
Unlike the daily oral tablets that have formed the backbone of HIV treatment for decades, Lenacapavir is administered as a subcutaneous injection only once every six months.
This biannual dosing schedule marks a significant shift from current antiretroviral therapies (ART) that require strict daily adherence, something that has long been a barrier to effective treatment in many resource-limited settings.
For Kenya, the drug represents more than just a scientific breakthrough; it offers hope for transforming how HIV is managed at a national level.
The government has invested heavily in the fight against HIV, with international partners like PEPFAR and the Global Fund providing substantial support.
However, challenges persist, including drug stockouts, logistical bottlenecks in ART distribution, and widespread issues with treatment adherence, particularly among young people and marginalised populations.
Kenya will introduce the drug alongside nine African nations selected to pioneer its rollout by January 2026.
Other countries are Eswatini, Lesotho, Mozambique, Nigeria, South Africa, Uganda, Zambia, and Zimbabwe.
Health Cabinet Secretary, Aden Duale, has thrown full weight behind the rollout of the ground-breaking drug, announcing that an implementation plan crafted through close collaboration with key stakeholders is already in place.
“This milestone underscores our collective determination to expand access to effective, discreet, and sustainable prevention options across the region,” Duale declared, emphasising the drug’s potential to reshape HIV treatment in Kenya and beyond.
The CS has vowed the government’s unwavering commitment to making Lenacapavir accessible to all who need it, with a sharp focus on reaching priority groups through strong community engagement.
“Integration of the new drug into our national HIV response strategy will reaffirm our commitment to equity, innovation, and community-led health solutions,” he said.
With just two injections per year, patients are less likely to miss doses, potentially reducing the rate of treatment failure and drug resistance.
This also translates into fewer clinic visits, which not only benefits patients, many of whom must travel long distances to access care, but also relieves pressure on overburdened healthcare workers and facilities.
Moreover, from a public health perspective, improving adherence and viral suppression rates means a lower risk of onward transmission.
Kenya is striving to achieve the UNAIDS 95-95-95 targets: 95 per cent of people living with HIV knowing their status, 95 per cent of those diagnosed receiving sustained ART, and 95 per cent of those on ART achieving viral suppression.
Another significant implication of Lenacapavir's introduction is the potential for cost savings in the long term.
While the initial cost of the drug may be higher than existing first-line therapies, the reduction in hospital admissions, clinic visits, and treatment of opportunistic infections could offset the expenditure.
For a government grappling with numerous public health priorities—ranging from non-communicable diseases to maternal health—Lenacapavir offers a strategic investment in a more sustainable HIV response.
There are, however, challenges to be addressed before Lenacapavir can be widely rolled out in Kenya and across Africa.
Health officials have cited supply chain integration, healthcare worker training, and community sensitisation as some of the challenges.
Affordability has also been cited as another pressing concern. Gilead has announced its commitment to ensuring global access through licensing agreements with generic manufacturers.
Nonetheless, health actors note that Kenya's strong history of successful ART programmes and community-based outreach initiatives positions the country well to pilot and scale the use of Lenacapavir.
The Ministry of Health, in partnership with organisations like NASCOP (National AIDS and STI Control Programme), is reportedly in advanced discussions about including the drug in its national treatment guidelines once all regulatory hurdles are cleared.
In the broader African context, Lenacapavir’s arrival signals a new era in HIV management—one that shifts from daily survival to long-term stability.
It reinforces the principle that people living with HIV should not merely live longer but live better, with more dignity, fewer disruptions, and reduced stigma.
“For Kenya and countries across the continent, the challenge now lies in harnessing the new innovation efficiently and equitably,” a doctor who spoke to the Star on anonymity said.
He emphasised that if the drug is successfully integrated, Lenacapavir could do more than lower viral loads; lighten the economic and psychological load borne by millions and mark a turning point in Africa’s decades-long fight against HIV/AIDS.





Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!