
A growing wave of drug-resistant infections is complicating wound care across Kenya, with health experts warning that continued reliance on “trial-and-error” treatment is putting patients at risk and delaying healing.
A new medical commentary by Dr Silas Awuor, a microbiologist at Jaramogi Oginga Odinga Teaching and Referral Hospital (JOOTRH), paints a troubling picture of wound management in the country—one in which antibiotics are often prescribed without proper laboratory testing, even as resistance to common drugs soars.
According to the report, resistance to widely used antibiotics such as ampicillin and cotrimoxazole has exceeded 90 per cent in some cases, rendering them largely ineffective in treating infections.
This, combined with the rise of hard-to-treat bacteria such as methicillin-resistant Staphylococcus aureus (MRSA), is complicating recovery for patients with acute and chronic wounds.
“Wound care in Kenya is still largely empirical,” Dr Awuor said, referring to treatment decisions made without laboratory confirmation of the specific bacteria involved.
“This disconnect between clinical practice and microbiological evidence is undermining treatment effectiveness and accelerating antimicrobial resistance.”
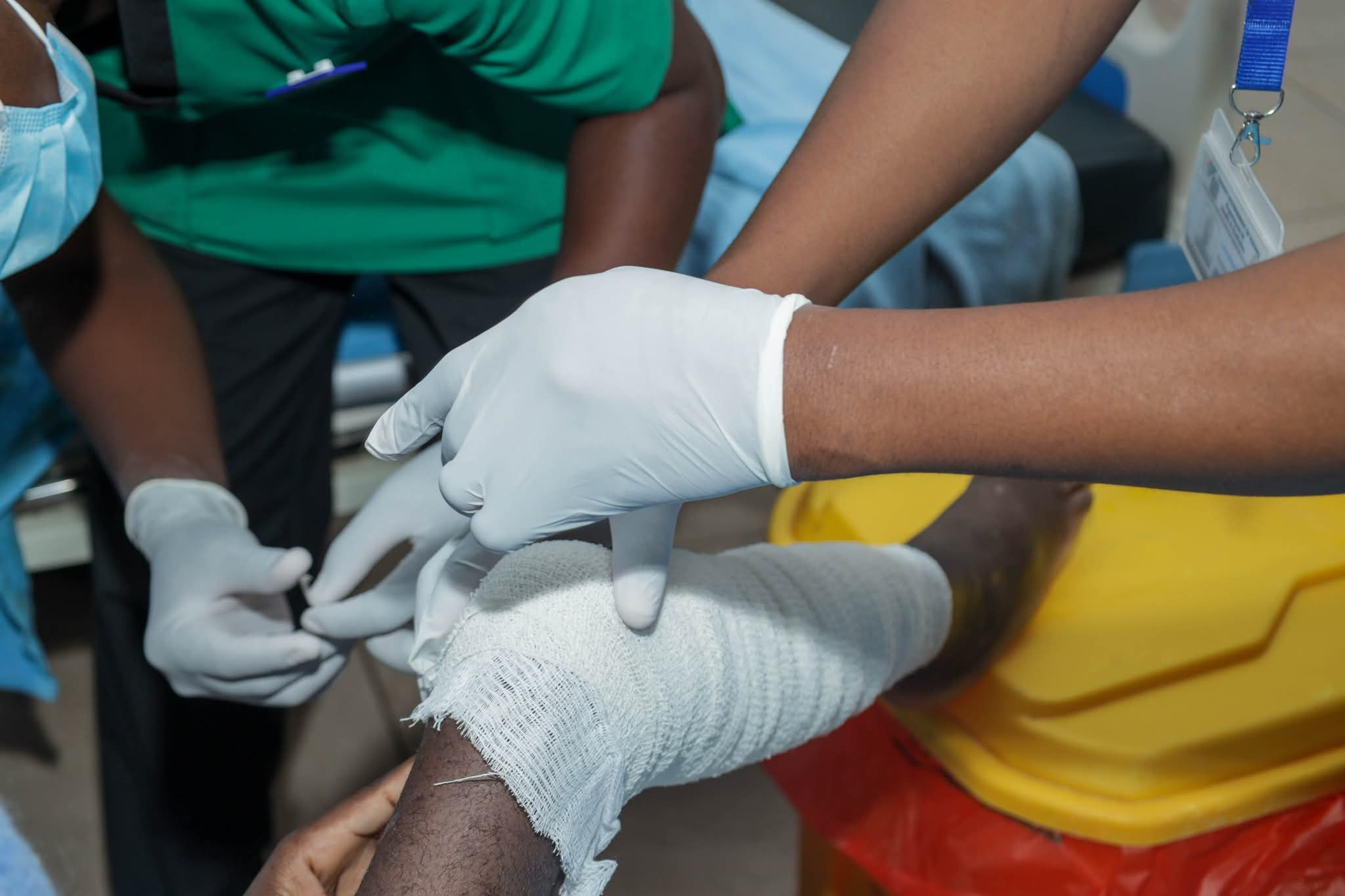
Wound infections, including surgical site infections, trauma-related wounds, and chronic conditions such as diabetic foot ulcers, are a major contributor to illness and rising healthcare costs in the country.
In many facilities, clinicians prescribe antibiotics based on experience rather than test results—a practice that experts say is no longer sustainable in the face of evolving resistance.
While Kenya has made strides in developing innovative and affordable wound care methods, such as honey-based dressings and improvised negative pressure therapy, the microbiological aspect remains largely neglected.
This gap, the report argues, is a key factor behind persistent infections and prolonged healing.
Studies conducted in hospital settings, particularly in Kisumu county, reveal that many wounds are infected by multiple types of bacteria, often with strong resistance to commonly used drugs.
These bacteria not only survive treatment but can also form biofilms—protective layers that shield them from antibiotics and the body’s immune system.
Biofilms are now believed to be present in a significant number of chronic wounds, making infections more difficult to eliminate.
Patients with such infections often experience delayed healing, repeated hospital visits and, in severe cases, complications that may lead to amputation or death.
The report highlights antimicrobial resistance (AMR) as a growing global crisis, with sub-Saharan Africa bearing a disproportionate burden.
In Kenya, limited access to diagnostic services and weak integration between laboratory findings and clinical decisions have worsened the situation.
“Even where laboratory services exist, the results are not always used to guide treatment,” the report notes. “This leads to inappropriate antibiotic use and missed opportunities for targeted care.”
To address these challenges, experts are calling for a shift towards what is known as microbiological stewardship— a more evidence-based approach to wound care that prioritises early diagnostic testing, targeted therapy and closer collaboration between clinicians and laboratory specialists.
Under this approach, patients would undergo culture and sensitivity testing early in the treatment process to identify the exact bacteria causing infection and determine which antibiotics are most effective.
This would not only improve patient outcomes but also reduce the misuse of antibiotics, a major driver of resistance.
Additionally, healthcare providers are encouraged to adopt strategies that disrupt biofilms, such as proper wound cleaning and debridement, alongside antibiotic treatment. Without addressing these protective bacterial structures, experts warn, even the most potent drugs may fail.
The report also calls for the development of facility-specific treatment guidelines based on local data, known as antibiograms, to help clinicians make informed decisions tailored to their environment.
Training and capacity-building for healthcare workers, as well as improved coordination between departments, are also seen as critical steps towards improving wound care outcomes.
“The future of wound care in Kenya depends not only on innovation but on integrating scientific evidence into everyday practice,” Dr Awuor said.
“Moving away from guesswork to targeted, data-driven treatment is essential if we are to win the fight against antimicrobial resistance.”
As Kenya continues to grapple with the broader impact of drug-resistant infections, the findings serve as a stark reminder that the battle lies not only in developing new treatments but also in using existing ones wisely.






Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!