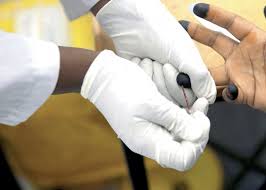
 Fewer Kenyans are testing for HIV./HANDOUT
Fewer Kenyans are testing for HIV./HANDOUTThe number of Kenyans tested for HIV fell after the US briefly suspended health funding to Kenya and other countries last year, according to figures released by the US State Department.
The data also shows a decline in the number of Kenyans diagnosed with and treated for HIV last year.
This has raised concerns that thousands of infections are now going undetected and untreated.
The department released figures for previous years and only for the last quarter of 2025 because funding had been suspended in the first months of 2025.
In the last quarter of 2024, Kenya, with support from the US President’s Emergency Plan for AIDS Relief (Pepfar), tested about 5,688 people for HIV. That figure fell to 5,539 in the last quarter of 2025.
Experts say the decline may appear modest in isolation, but it reflects a wider and more troubling disruption across the system.
As testing fell, the number of people diagnosed with HIV also declined, dropping from about 5,319 to 4,754 over the same period.
Health advocates caution that this does not signal a reduction in infections, but rather a growing pool of undiagnosed cases.
“Testing is the front door of the HIV response,” said Nelson Otwoma, head of Nephak, the network of Kenyans living with HIV.
“When fewer people walk through that door, the entire system begins to weaken.”
The number of people newly initiated on treatment also dropped sharply, from about 776 in late 2024 to 646 in late 2025, a fall of nearly 17 per cent.
This suggests that even among those who are diagnosed, fewer are being rapidly enrolled in life-saving care.
A spokesperson for the US State Department addressed the global decline in children diagnosed with HIV, saying it reflects progress in reducing mother-to-child transmission, consistent with historical trends.
“These declines are expected to continue, particularly with US government funding of Lenacapavir, which can further prevent mother-to-child transmission,” the office of Tammy Bruce said in a statement.
President Donald Trump suspended almost all US foreign aid for 90 days when he came to office in January last year.
Most prevention efforts, including testing and pre-exposure prophylaxis, were curtailed.
Although services were later allowed to resume, the interruption fractured the complex network of clinics, outreach workers, supply chains and community programmes that sustain HIV services across Kenya.
The National AIDS and STI Control Programme says Kenya relies on HIV testing as the main entry point to prevention, care, support and treatment services.
“HIV testing and counselling is central to all HIV programmes nationwide and is closely linked with other health services,” Nascop says in its National Guidelines for HIV Testing and Counselling in Kenya.
The new data, released on April 17, suggests that Kenya has so far managed to maintain treatment for those already enrolled in care.
This aligns with global observations that long-term patients, often linked to government-run facilities, are less immediately affected by funding shocks.
However, experts warn that this stability can be misleading. Without strong testing and diagnosis rates, the pipeline of new patients entering care shrinks.
Over time, this creates conditions for a resurgence of the epidemic, as untreated individuals continue to transmit the virus unknowingly.
In December last year, Kenya and the United States signed a five-year agreement to replace health funding from Pepfar.
The deal, signed by US Secretary of State Marco Rubio and Prime Cabinet Secretary Musalia Mudavadi, committed the United States to provide up to $1.6 billion (Sh207 billion) over five years.
In return, Kenya must raise about $850 million in domestic resources over the same period.
Kenya will receive a large portion of the Sh207 billion grant first, but the amount will reduce each year until 2031, when Kenya is expected to fully finance its HIV treatment, prevention and other health services.
This grant replaced all Pepfar (US President’s Emergency Plan for AIDS Relief) funding to Kenya and all other health financing that previously came through USAID each year.
Pepfar has been the backbone of Kenya’s HIV response for two decades, supporting antiretroviral treatment for more than 1.3 million people and financing critical health workers, commodities and community programmes.






Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!