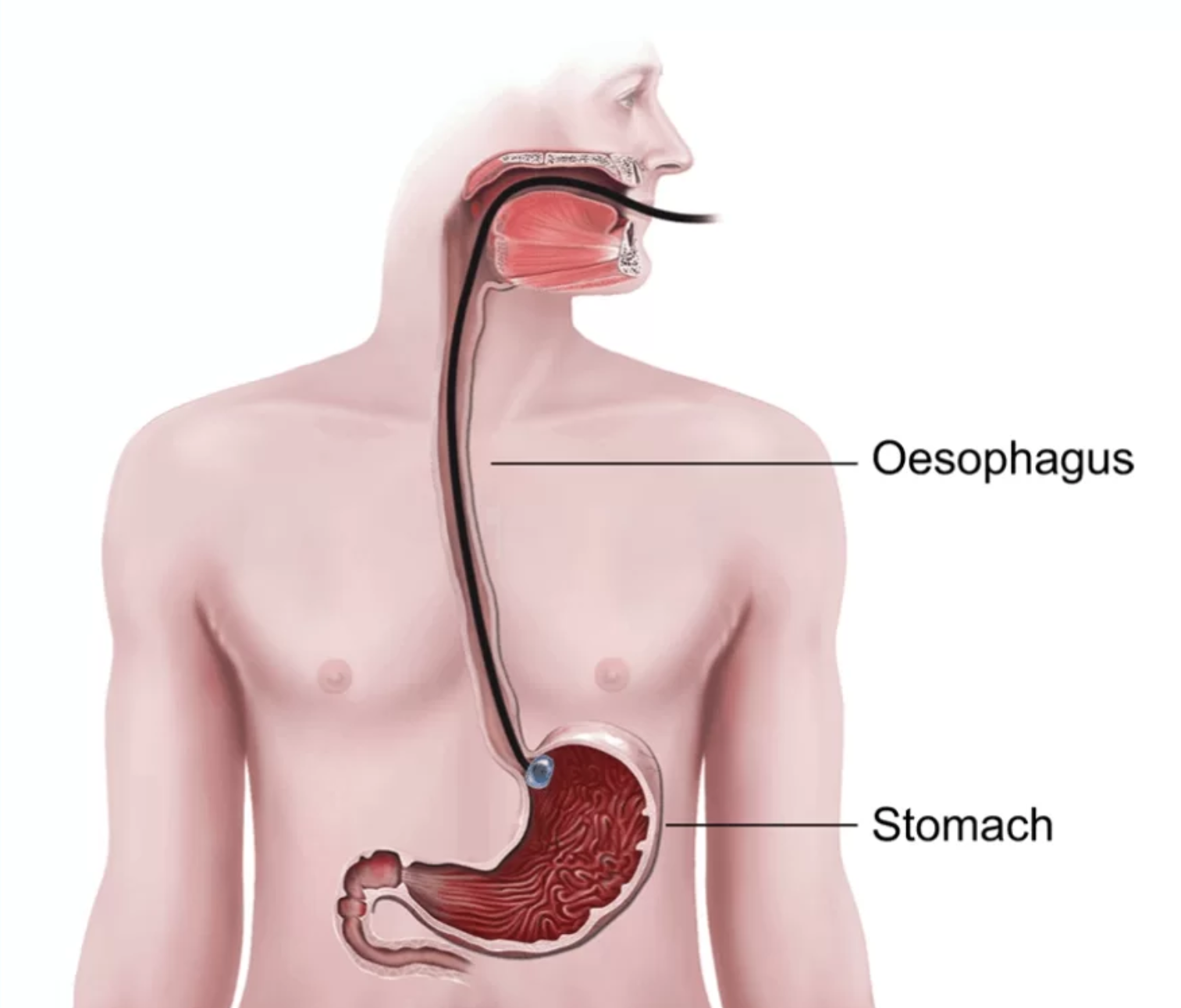
 The oesophagus: Surgeons at Kenyatta National Hospital (KNH) carry out the surgeries, allowing children to eat again.
The oesophagus: Surgeons at Kenyatta National Hospital (KNH) carry out the surgeries, allowing children to eat again.Surgeons typically prefer to pull up the stomach into the chest or neck to replace a missing or damaged oesophagus.
But if the stomach is unsuitable for use, they cut a section of the patient’s own large intestine (colon) and stitch it into place to serve as a brand-new food pipe (oesophagus).
Dr Brian Bichanga, a surgeon from the University of Nairobi’s Department of Paediatric Surgery, and colleagues looked at four children and young adults who underwent this complex surgery at the Kenyatta National Hospital, as early as 20 years ago.
Their findings, published in the Pan African Medical Journal, reveal that while the surgery (known as colon interposition) is life-saving, many patients face lasting health and emotional challenges.
“Colon interposition remains a valuable option for oesophageal replacement in complex pediatric and young adult cases. However, long-term functional and nutritional outcomes remain variable,” they wrote.
The colon is more preferred to other types of replacements because it is naturally resistant to the harsh acids of the stomach and often lasts longer.
Dr Bichanga’s team studied four patients who had this surgery between 2014 and 2019. Two were born with long-gap oesophageal atresia. Two burned their food pipes after swallowing corrosive substances such as cleaning materials in containers such as soda bottles.
All of them experience complications after the surgery.
“Strictures were the most common complication, observed in three out of four patients, one of whom required surgical revision. Similar challenges have been documented from other studies,” the researchers reported.
A stricture is a narrowing where tissues are joined together. It led to difficulty swallowing in these patients, repeated hospital visits and, in some cases, dependence on feeding tubes.
One three-year-old boy born with oesophageal atresia developed a tight narrowing and reflux after the surgery. He can now take mostly semi-solid and liquid foods. An 11-year-old boy who swallowed a caustic substance still depends largely on a tube placed into his stomach for feeding.
Growth was also uneven. Two patients had normal height and weight for their age. Two were stunted or severely underweight, including a 23-year-old woman who had her surgery at age two and remains significantly shorter and thinner than average.
Quality of life scores told a more complex story as three of the four patients had lower emotional, social or school functioning scores.
Dr Bichanga and his colleagues emphasised that the surgery is only the beginning of care.
“Colon interposition can provide durable oesophageal continuity with satisfactory long-term function. Nonetheless, complications such as stricture, reflux, and impaired growth are common, underscoring the need for structured, long-term multidisciplinary surveillance,” they concluded.
The study is small, involving only four patients, and has no comparison group. However, they said it offers rare long-term data from a public hospital in Kenya, where children with these severe conditions are treated.
Their paper is titled, Long-term outcomes after colon interposition for oesophageal replacement: a case series of four patients from a single centre.





Comments 0
Sign in to join the conversation
Sign In Create AccountNo comments yet. Be the first to share your thoughts!